Vaginal Support Surgeries
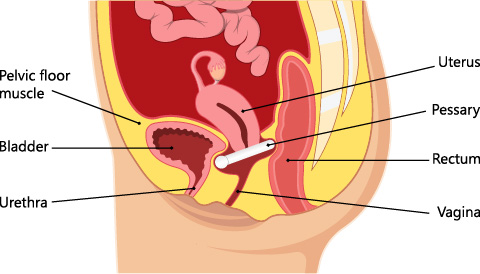
Pelvic relaxation is a broad and often complicated topic that refers to weakness in all or parts of the vagina. Patients often refer to these problems as “something falling out;” which may include the bladder, uterus, rectum, or the top of the vagina. Medical terms for these disorders include prolapse, cystocele, uterine prolapse or procidentia, rectocele, and enterocele.
They may occur as isolated defects, or in combination. Prolapse problems usually arise as a result of childbirth, but genetics and family history also often play an important role in the development of these problems.
By itself prolapse is not necessarily a problem, but when it causes symptoms such as pressure, bladder or bowel dysfunction, or the vagina literally falling out, treatment may be indicated. In laymen’s terms, these issues include urinary retention, leakage, frequent urinary tract infections, severe constipation, low back ache, a bulging mass protruding low or out of the vagina, and sexual discomfort.
Most of the time treatment will be a surgical procedure or a combination of surgical procedures to re-support the vagina and surrounding structures.
Some patients for personal reasons or because they are not healthy enough to go through surgery prefer to use a pessary. A pessary is a rubber or silastic type device, often shaped like a donut, that is placed in the vagina to hold, or push up protruding vaginal parts. It is left in the vagina most of the time.
The following discussion relates to surgical repair of prolapse.
Procedures
Often referred to as anterior (bladder) and posterior (rectum) and enterocele repair (top of the vagina) or colpopexy.
In current times most repairs of the vagina involve “mesh” or “graft” materials to reinforce weakened tissue. They are most commonly placed through vaginal incisions and attached to ligaments deep within the pelvis. The grafts may look like window screen material, and are used to lift up or push down protruding vaginal tissue. Sometimes laparoscopy of abdominal incisions may be used to assist in placement. A concomitant hysterectomy may also be necessary for best results.
For some patients, it may be necessary to re-support only part of the vagina; for other patients multiple grafts are required if there are multiple defects in the vagina.
The best aspect about graft procedures is that since we are using long lasting material, surgical correction of the defect(s) should be permanent. In the past surgical procedures for prolapse often failed, or “fell down” after several years.
Pre-procedure preparation
In general there is none other that routine preoperative workup and preparation. Sometimes we may ask you to perform a urodynamics test in the office. Postmenopausal patients are often asked to use a vaginal estrogen cream for several weeks or months prior to surgery to ensure optimal vaginal health and healing. Also because narcotics and anaesthesia can slow down the bowels and cause constipation and because we don’t want you to have to strain to evacuate we will ask you to take a laxative the day before the procedure to clean out your bowels.
Risks
Although most of the time the incisions are hidden in the vagina, these procedures are considered “major surgery.” Mesh grafts are permanent and meant to last forever. The most common risks include erosion or graft exposure, sexual discomfort, urinary retention, or increase in leakage, bleeding, infection, and damage to surrounding structures. Graft rejection is rare. Most studies quote complication rates of less than 5 – 10%, and are usually correctable with minor procedures.
Aftercare
Hospital stay is usually limited to one overnight stay. After discharge, the patient can usually resume simple daily activities such as bathing, walking, and regular diet immediately. On the other hand, most will need at least 2 weeks out of work, and strenuous activities such as exercise or sexual intercourse must be avoided for 6 weeks,
Many handouts with pictures, dvd’s, videos, and websites are available for review. In most cases however a thorough discussion with your healthcare provider is all that will be necessary to fully understand the overall scope of pelvic relaxation and the procedures for repair.
Let's stay in touch
Our monthly newsletter keeps you up-to-date on healthy lifestyle, latest news, and our practice.