Laparoscopy
Laparoscopy is a minimally invasive procedure to view your pelvic organs internally and address many gynecological problems. This is accomplished by using a fiber-optic camera passed through a tiny incision in the abdomen.
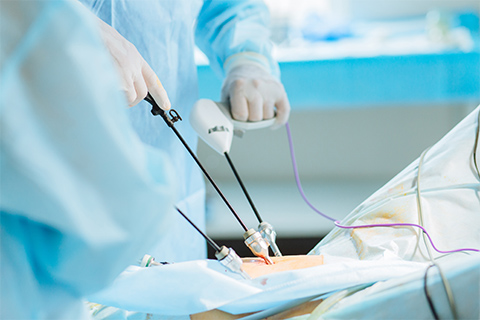
Laparoscopy is a minimally invasive procedure to internally view your pelvic organs and address many gynecological problems. This is accomplished by using a fiber-optic camera passed through a very small incision in the abdomen. Diagnostic laparoscopy is used to internally view the reproductive organs and assist in diagnosing a problem. It is useful in the evaluation of pelvic pain, examining a pelvic mass, diagnosing endometriosis or pelvic infections, and in infertility evaluation. Operative laparoscopy is when a problem is addressed such as removing a cyst, treatment of endometriosis, hysterectomy, tubal ligation or removing scar tissue.
Preoperative Preparation
We recommend not eating or drinking after midnight the night before your procedure. Your physician may request that you take a medicine or a bowel preparation the night before the procedure. If this is the case, please follow your physician’s instructions. We recommend wearing loose-fitting clothes to the surgery center or hospital, leaving jewelry at home and having someone drive you and pick you up for the procedure. You should arrive at the surgery center 1 ½ hours prior to the procedure or the hospital 2 hours prior to the procedure.
The Procedure
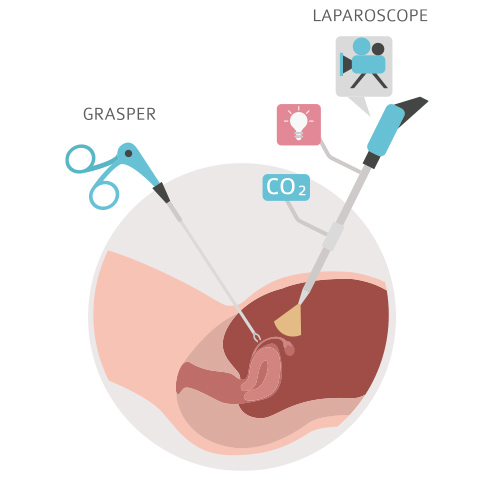
Your doctor will make one to four small incisions in your abdomen to perform the procedure. These incisions will be small, often less than a centimeter. You will be under general anesthesia. Following surgery, you will be in the recovery room for a short amount of time. Once you have recovered, you will be given discharge instructions and go home. If your procedure requires an overnight stay, you will be transferred to your room.
General risks of laparoscopy include damage to surrounding structures, pain, wound infection, bleeding which may or may not require transfusion, blood clot formation and having to make a bikini line incision to address any complication. We take every measure to minimize these surgical risks.
[Image Adapted from www.ovarian-cancer-facts.com]
Postoperative Expectations
Postoperatively you can anticipate abdominal soreness for 1-2 weeks, depending on the procedure performed. It is not uncommon to notice vaginal spotting postoperatively, and some women may experience menstrual irregularity including a missed period over the next 6 weeks. For the next 1-2 days, you may also experience abdominal swelling, pain or discomfort in the shoulder blade or neck region, a sore throat and occasional nausea. Sometimes taking a warm bath or using a heating pad can ease these symptoms. Do not drink alcohol for 1-2 days postoperatively or while you are taking narcotics. We recommend not driving while you are still on narcotics for pain relief. It is okay to shower at anytime postoperatively. If pathology is sent, you will either be contacted or your physician will discuss the results at your postoperative visit. Lastly, avoid sexual activity, tampons or douching for at least 1 week postoperatively.
When to Call
We are available 24 hours/day 7 days a week to address concerns. You should contact us for any of the following concerns:
- Pain not relieved by your narcotics
- Fever of 101 or greater
- Any redness, swelling or drainage from the incision sites
- Vaginal bleeding soaking more than 1 sanitary pad in two hours
- Persistent nausea and/or vomiting for more than 24 hours post operatively
Let's stay in touch
Our monthly newsletter keeps you up-to-date on healthy lifestyle, latest news, and our practice.