Amniocentesis
Amniocentesis is the most accurate method for detecting chromosomal abnormalities. It is also used to identify fetuses affected by inherited genetic disorders like cystic fibrosis, Tay-Sachs disease, or sickle cell anemia. Other uses include detecting spina bifida and determining fetal lung maturity.
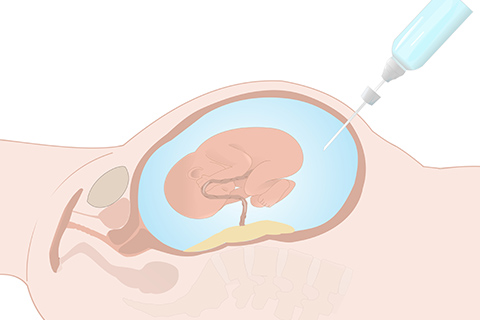
In this procedure, a sample of amniotic fluid is removed and analyzed. Fetal cells freely floating in amniotic fluid are grown in culture and chromosomal data is extracted. This process can take up to 2 weeks. Proteins in amniotic fluid serve as biochemical markers that help us evaluate fetal lung maturity and search for conditions like spina bifida. Occasionally, the doctor is unable to extract fluid from the uterus due to a variety of technical reasons or the cells fail to grow in the lab. In both of these situations, the procedure can be repeated.
During amniocentesis, fluid is removed by placing a long thin needle through the abdominal wall into the amniotic sac. The amniocentesis needle is guided into the sac with the help of ultrasound imaging performed prior to and during the procedure. Once the needle is in the sac, a syringe is used to withdraw the amniotic fluid containing fetal cells, proteins and fetal urine. The fluid is usually straw-colored resembling dilute urine. The volume of fluid withdrawn depends upon the age of the fetus and the reason for the testing. We usually require 20cc of fluid.
For most patients, amniocentesis is a fairly quick and comfortable procedure. Some women experience some uterine cramping or a feeling of faintness.
We ask that all of our patients coming in for amniocentesis arrive with a support person who can drive them home. We also ask that for the first 24 hours after amniocentesis, our patients rest, not return to work, avoid exercise, and not fly.
If you experience severe persistent cramping, bleeding, leakage of fluid, or abdominal or uterine tenderness more than mild cramping and discomfort from the needle site call our office for evaluation.
Let's stay in touch
Our monthly newsletter keeps you up-to-date on healthy lifestyle, latest news, and our practice.